Home HBOT
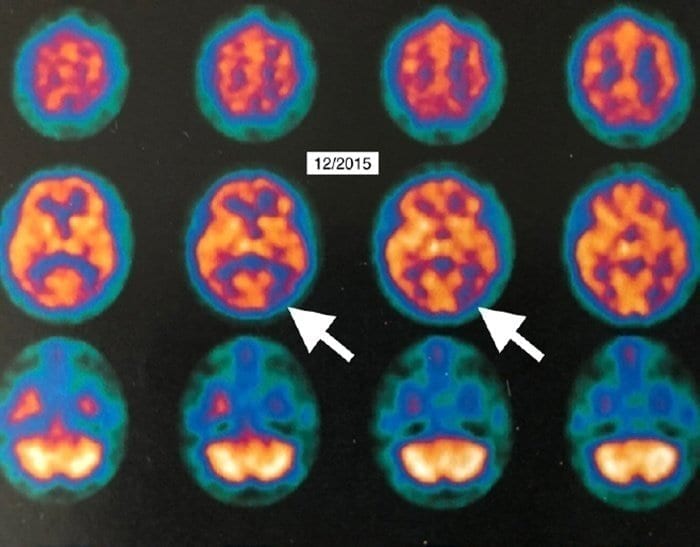
Dr. Paul Harch, Clinical Professor and Director of Hyperbaric Medicine at LSU Health New Orleans School of Medicine, and Dr. Edward Fogarty, Chairman of Radiology at the University of North... Read more
Certified scuba divers are familiar with the use of hyperbaric oxygen therapy (HBOT) for decompression sickness treatment. However, in the past 50 years, researchers have revealed HBOT’s bro... Read more